Hypertonic Pelvic Floor: When Pelvic Muscles Stay Too Tight
Persistent pelvic discomfort often leaves people searching for answers that never seem to appear in routine medical conversations. Pain during intimacy, unexplained urinary urgency, or a constant sense of pelvic tension can feel confusing and isolating. Many individuals spend years treating symptoms rather than identifying the muscular imbalance at the root of the problem.
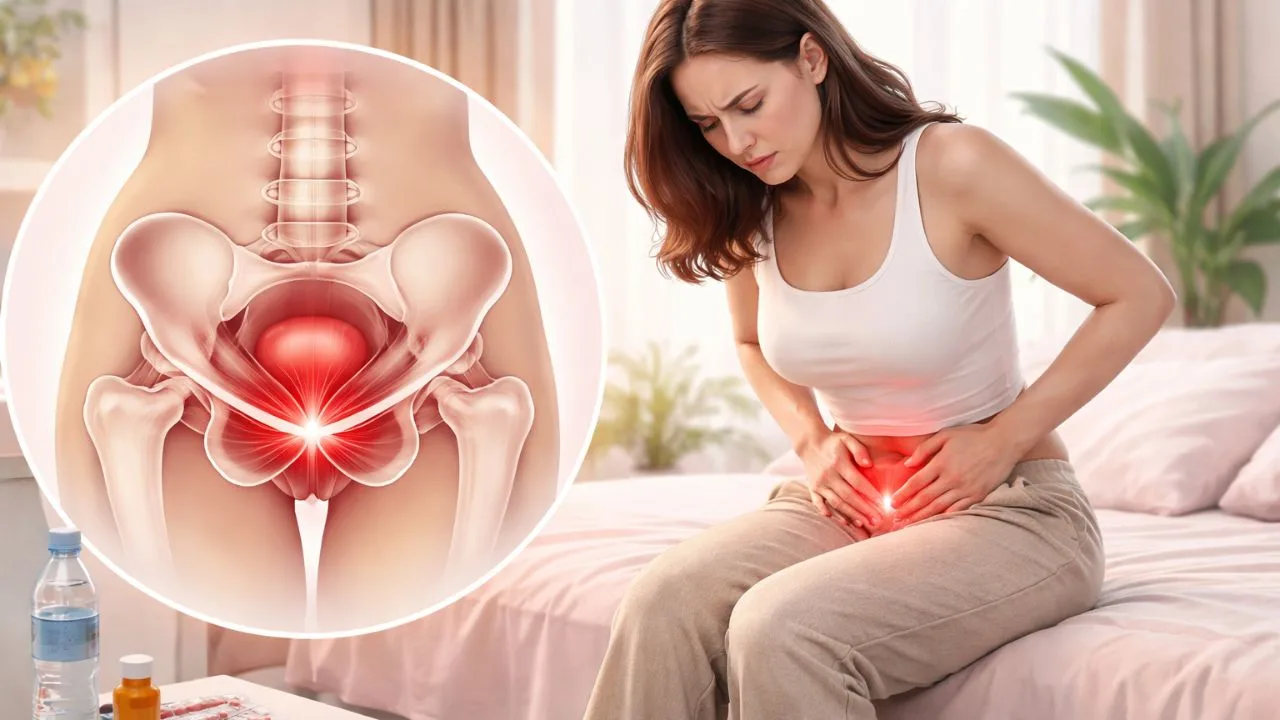
One condition frequently hidden beneath these experiences is hypertonic pelvic floor. The pelvic floor consists of a group of muscles that support organs such as the bladder, uterus, prostate, and rectum. When those muscles remain excessively tight or unable to relax, the system becomes dysfunctional rather than supportive.
Clinical pelvic health specialists increasingly recognize this condition as a major contributor to chronic pelvic pain, bladder problems, bowel difficulties, and sexual discomfort. The issue rarely receives attention in general health discussions even though pelvic muscle tension affects people of every gender and age group.
The following exploration examines what hypertonic pelvic floor means, why the condition develops, how symptoms appear in daily life, and how modern pelvic therapy approaches help restore healthy muscle function.
What Hypertonic Pelvic Floor Means in Muscular and Functional Terms
The pelvic floor acts as a supportive hammock stretching between the pubic bone and tailbone. This muscle network maintains continence, stabilizes the spine, assists breathing mechanics, and contributes to sexual function. Healthy pelvic muscles contract when needed and relax when the body requires release.
Hypertonic pelvic floor occurs when these muscles remain in a constant state of contraction. Rather than responding dynamically, the tissue holds excessive tension similar to a clenched fist that never opens. Over time this tension reduces circulation, increases nerve sensitivity, and disrupts coordination with surrounding muscles.
Pelvic floor muscles share neurological connections with the diaphragm, abdominal wall, and deep spinal stabilizers. When tension persists in one region, the entire pressure management system of the body becomes disrupted. This explains why individuals with pelvic floor tension frequently experience back pain, hip discomfort, or breathing dysfunction.
Medical literature often describes this condition using related terms such as nonrelaxing pelvic floor dysfunction, pelvic floor overactivity, or high tone pelvic floor. Despite variations in terminology, the underlying mechanism remains the same. Muscles that should relax during urination, bowel movements, or intimacy remain excessively contracted.
How Muscle Tone Becomes Pathologically Elevated
Muscle tone represents the baseline tension present in resting muscle tissue. Normal tone allows muscles to react quickly and maintain structural support. Excess tone, though, creates rigidity and fatigue.
Pelvic muscles become hypertonic when the nervous system continuously signals contraction. This may occur through stress responses, protective guarding after injury, or habitual postural patterns. Over time the brain begins to interpret tension as the normal resting state.
A significant factor involves neuromuscular miscommunication. The pelvic floor receives signals from the pudendal nerve and sacral nerve roots. When pain or trauma affects this system, muscle guarding often develops as a protective mechanism.
The protective response becomes problematic once the original trigger disappears but the tension pattern remains. Many individuals unknowingly maintain pelvic clenching throughout the day while sitting, exercising, or even sleeping.
The Difference Between Hypertonic and Hypotonic Pelvic Floor
Public discussions about pelvic health frequently focus on weak pelvic muscles. That condition, known as hypotonic pelvic floor, results in reduced support and possible incontinence.
Hypertonic pelvic floor represents the opposite imbalance. Instead of weakness, the muscles become excessively tight and unable to lengthen. Ironically both conditions may produce similar symptoms such as urinary difficulty or pelvic discomfort.
Distinguishing between the two is crucial for treatment. Strengthening exercises like traditional pelvic contractions can worsen hypertonic conditions by increasing tension in already overactive muscles.
A careful evaluation by pelvic health professionals helps determine the muscle tone pattern before any therapeutic exercises begin.
Symptoms That Suggest Pelvic Floor Muscle Overactivity
The body rarely presents pelvic floor tension through a single symptom. Instead individuals often report a cluster of discomforts that seem unrelated until a pelvic evaluation connects the dots.
Chronic pelvic pain appears among the most common complaints. The sensation may feel like pressure, burning, or deep muscular aching within the pelvis, lower abdomen, or tailbone area. Pain intensity often fluctuates throughout the day depending on posture or stress levels.
Urinary symptoms frequently accompany muscle overactivity. Difficulty starting urination, a sensation of incomplete emptying, or frequent urges without significant bladder volume can signal pelvic floor dysfunction.
Sexual discomfort also appears in many patients with hypertonic pelvic muscles. Penetration pain, erectile difficulties, or post orgasm discomfort can arise from excessive muscle tension and reduced blood flow in pelvic tissues.
Bladder and Urinary Complications Linked to Pelvic Tension
The pelvic floor coordinates closely with bladder function. Muscles must relax fully for the bladder to empty properly. When hypertonicity prevents relaxation, urinary flow becomes restricted.
Individuals sometimes describe standing at the toilet waiting for urine to begin while sensing pelvic tightness. Others notice interrupted urine streams or repeated urges soon after voiding.
This pattern often leads patients to suspect urinary tract infections even though laboratory testing shows no infection present. The underlying issue lies within muscular coordination rather than the urinary system itself.
Long term tension may also contribute to bladder sensitivity. Constant pressure on bladder nerves increases the feeling of urgency even when bladder volume remains small.
Bowel Dysfunction and Digestive Discomfort
The pelvic floor plays a vital role during bowel movements. Muscles must lengthen and release to allow stool passage. Hypertonicity interferes with this natural relaxation process.
Individuals experiencing pelvic floor tension often report constipation that does not respond to dietary fiber or hydration changes. Straining during bowel movements may become routine due to restricted muscular opening.
The effort involved can create additional pelvic pressure, reinforcing muscle guarding and perpetuating the cycle of dysfunction.
Digestive specialists increasingly collaborate with pelvic therapists when chronic constipation appears alongside pelvic discomfort. This collaborative approach helps identify muscular restrictions that traditional gastrointestinal treatments overlook.
Why Hypertonic Pelvic Floor Develops
Several pathways can lead to pelvic floor overactivity. Physical trauma, emotional stress, postural strain, and repetitive muscular patterns all influence pelvic muscle tone.
Psychological stress deserves particular attention. The pelvic floor participates in the body’s fight or flight response. During stress the nervous system signals muscles to contract protectively. Chronic stress therefore encourages sustained pelvic tension.
Athletic training sometimes contributes as well. High intensity abdominal workouts, heavy lifting, or sports requiring strong core bracing can create persistent pelvic muscle engagement if relaxation techniques are absent.
Past pelvic injuries, childbirth trauma, or surgical procedures may also trigger protective muscle guarding. Even after tissue healing occurs, the nervous system may maintain defensive contraction patterns.
Postural Habits and Sedentary Lifestyle
Modern lifestyles involve extended sitting at desks or driving vehicles. Prolonged sitting compresses the pelvic region and limits blood circulation within pelvic tissues.
When individuals maintain seated positions for hours while unconsciously clenching abdominal or pelvic muscles, the tissues gradually adapt to that shortened position.
Over months or years the pelvic floor loses its natural elasticity. Standing or walking may then trigger discomfort because the muscles resist lengthening.
Postural imbalance involving the hips, spine, and diaphragm further contributes to pelvic tension. The pelvic floor works in coordination with these structures. Dysfunction in one region often influences the others.
Emotional Trauma and Nervous System Patterns
Pelvic muscles contain strong connections to emotional processing within the nervous system. Experiences involving fear, pain, or trauma frequently lead to unconscious muscular guarding in the pelvic region.
Psychological stress increases sympathetic nervous system activity. This heightened state encourages muscle contraction and reduces relaxation signals.
Patients sometimes report pelvic symptoms emerging during stressful life periods even without physical injury. The nervous system interprets emotional distress as a signal for protective muscular tightening.
Pelvic therapy approaches increasingly incorporate nervous system regulation techniques such as breathing retraining and somatic awareness to address this component.
Clinical Evaluation and Diagnosis
Diagnosing hypertonic pelvic floor requires a detailed assessment by clinicians trained in pelvic health. Many primary care settings lack specialized evaluation techniques, which explains why patients often move through multiple consultations before receiving an accurate diagnosis.
The evaluation typically begins with a thorough history exploring symptoms related to urination, bowel movements, sexual function, and musculoskeletal pain. Patterns within these experiences often reveal underlying pelvic dysfunction.
Physical examination includes external observation of posture, breathing mechanics, and hip mobility. These factors influence pelvic floor behavior.
Internal pelvic assessment performed by trained clinicians allows direct evaluation of muscle tone, trigger points, and coordination during contraction and relaxation.
Muscular Trigger Points and Pain Mapping
Hypertonic pelvic floor often involves myofascial trigger points within pelvic muscles. These localized areas of muscle tension can reproduce pain when pressure is applied.
During evaluation clinicians may gently palpate specific pelvic muscles to identify sensitive areas. Patients frequently recognize the sensation as similar to their daily discomfort.
Mapping these trigger points helps guide therapeutic strategies. Targeted manual therapy techniques often focus on releasing these restricted areas.
Pain mapping also assists in distinguishing pelvic floor dysfunction from other conditions such as bladder inflammation or gastrointestinal disorders.
Diagnostic Overlap With Other Pelvic Conditions
Several medical conditions share symptoms with pelvic floor tension. Interstitial cystitis, endometriosis, prostatitis, and irritable bowel syndrome sometimes coexist with pelvic muscle dysfunction.
A multidisciplinary evaluation helps identify whether muscle overactivity contributes to the symptom picture. Treating the muscular component often reduces overall symptom intensity even when other conditions remain present.
Collaboration between gynecologists, urologists, gastroenterologists, and pelvic therapists improves diagnostic accuracy and treatment outcomes.
Practical Reference Table for Pelvic Floor Function Indicators
|
Indicator |
Normal Pelvic Function |
Hypertonic Pelvic Floor |
Functional Impact |
Clinical Observation |
|
Muscle Resting Tone |
Balanced tension |
Persistent tightness |
Reduced relaxation |
Palpable rigidity |
|
Urination Pattern |
Smooth start and flow |
Delayed or interrupted stream |
Incomplete emptying sensation |
Pelvic contraction during voiding |
|
Bowel Movement |
Relaxed muscle release |
Difficulty relaxing muscles |
Straining and constipation |
Resistance during exam |
|
Sexual Function |
Comfortable muscular response |
Pain or tightness |
Reduced pleasure and discomfort |
Trigger point sensitivity |
|
Breathing Coordination |
Diaphragm and pelvis move together |
Restricted pelvic descent |
Shallow breathing pattern |
Limited pelvic mobility |
|
Pain Presentation |
Minimal baseline discomfort |
Chronic pelvic ache or pressure |
Activity related pain spikes |
Tender muscle bands |
Therapeutic Strategies That Restore Pelvic Muscle Balance
Treatment focuses on teaching pelvic muscles to release excessive tension. Pelvic health physical therapy remains one of the most widely recommended approaches.
Therapists trained in pelvic rehabilitation guide patients through relaxation exercises, manual therapy techniques, and movement retraining designed to restore muscular balance.
Breathing patterns play an important role in therapy. The diaphragm and pelvic floor move together during inhalation and exhalation. Coordinating this movement encourages natural pelvic relaxation.
Manual therapy often addresses trigger points and fascial restrictions. Gentle internal or external techniques gradually reduce muscular tension and improve circulation within pelvic tissues.
Movement Retraining and Functional Integration
Pelvic muscles function within the broader core system of the body. Therapy frequently includes retraining of posture, hip mobility, and spinal stabilization.
Activities such as walking mechanics, sitting posture, and lifting patterns may be adjusted to reduce unconscious pelvic clenching.
Patients often discover that daily habits contribute significantly to pelvic tension. Conscious relaxation during routine movements helps reprogram neuromuscular patterns.
Gradual integration of low load core exercises strengthens coordination without increasing muscle tone excessively.
Nervous System Regulation and Stress Response
Because pelvic tension often reflects nervous system stress patterns, therapeutic programs may include relaxation techniques aimed at reducing sympathetic activation.
Slow breathing practices, mindfulness based movement, and gentle stretching can calm the nervous system while encouraging pelvic muscle release.
Many patients notice symptom improvement when psychological stress decreases. Addressing emotional wellbeing becomes part of the healing process alongside physical therapy.
Long Term Outlook and Pelvic Health Maintenance
Recovery from hypertonic pelvic floor varies depending on symptom duration and underlying triggers. Individuals who begin therapy soon after symptom onset often experience faster improvement.
Chronic cases may require longer periods of neuromuscular retraining. The nervous system needs time to recognize that relaxation is safe after years of guarding patterns.
Regular movement, balanced exercise routines, and stress management strategies help maintain pelvic muscle health.
Education also plays a crucial role. Many patients report significant relief once they understand how pelvic muscles interact with breathing, posture, and emotional stress.
Healthcare awareness surrounding pelvic floor conditions continues expanding. Greater recognition allows earlier diagnosis and more targeted therapy for individuals experiencing pelvic discomfort.
Frequently Asked Questions
What does hypertonic pelvic floor feel like during daily activities?
Many individuals describe a constant sensation of tightness or pressure deep in the pelvis. Sitting for extended periods may increase discomfort, and activities such as urination or bowel movements can feel strained or incomplete. Some people notice pain radiating toward the hips or lower back, especially after physical exertion or stressful situations.
Can men develop hypertonic pelvic floor problems?
Yes. Pelvic floor tension affects men as well as women. Men often experience symptoms such as pelvic pain, urinary difficulty, or discomfort around the prostate region. Conditions sometimes labeled chronic prostatitis may actually involve pelvic floor muscle overactivity rather than infection.
Does stress contribute to pelvic floor tension?
Stress influences the nervous system and muscle tone throughout the body. The pelvic floor participates in protective responses during stressful situations. Persistent stress can therefore maintain chronic muscular contraction in the pelvic region, leading to symptoms associated with hypertonic pelvic floor.
Are traditional pelvic strengthening exercises helpful for this condition?
Strength focused pelvic exercises may increase symptoms when muscles already remain excessively tight. Pelvic therapists usually emphasize relaxation training, breathing coordination, and gentle lengthening techniques before introducing strengthening movements.
How long does pelvic floor therapy usually take?
Treatment duration varies widely depending on the severity of muscle tension and contributing factors. Some individuals notice improvements within several therapy sessions, while chronic cases may require several months of guided rehabilitation to restore normal muscle tone and coordination.
Can hypertonic pelvic floor resolve without treatment?
Mild cases sometimes improve through stress reduction, movement changes, and awareness of pelvic clenching habits. Persistent symptoms often require specialized pelvic therapy to release trigger points and retrain neuromuscular patterns.
Closing Perspective
Pelvic muscle health influences bladder control, bowel function, sexual comfort, and spinal stability. Hypertonic pelvic floor disrupts each of these systems through persistent muscular tension and nervous system imbalance. Recognizing the condition transforms confusing symptoms into a treatable muscular issue rather than a mysterious pelvic disorder.
Modern pelvic rehabilitation approaches continue revealing how breathing mechanics, emotional stress, posture, and muscular coordination shape pelvic function. When these elements align, the pelvic floor regains its natural rhythm of contraction and relaxation, restoring comfort and functional stability throughout daily life.