
Clinic margins feel tight because revenue leaks hide in plain sight. If you’re searching for physician billing services, you likely battle coding errors, modifier confusion, and slow denials. Here’s the fix. A specialty partner aligns front-end checks with clean claims and rigorous follow-up. You get fewer rejections, faster payments, and clear KPIs. In this guide, see what a physician billing company delivers, how it compares to in-house teams, and the exact steps to improve results in 90 days—so you can act with confidence.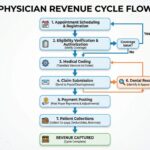
Why Physician Billing Breaks (And How to Fix It)
Small gaps stack into big revenue loss:
- Eligibility or auth errors cause avoidable denials.
- E/M level selection and modifier 25 misfires trigger audits.
- Missing diagnosis specificity blocks medical necessity.
- Place-of-service and telehealth rules change payment outcomes.
- Weak denial follow-up lets AR age out.
Tighten each step, and cash moves. Use data to prevent repeat issues.
What Are Physician Billing Services? (Definition)
Physician billing services manage the full claim life cycle for professional services. Teams verify coverage, capture charges, code encounters, scrub claims, submit to payers, chase denials, post payments, and track underpayments. Strong services add front-end checks, compliance reviews, and reporting that lifts clean-claim rates and cuts days in AR across specialties.
What Is a Physician Billing Company? (Definition)
A physician billing company brings certified coders, denial experts, and payer-specific knowledge. It integrates with your EHR and clearinghouse, applies payer edits pre-submission, manages appeals fast, and delivers dashboards by provider, location, and payer. The team also trains staff on documentation and modifier use to prevent repeat denials.
RCM vs Physician Billing Services (Definition)
Revenue Cycle Management (RCM) spans scheduling, eligibility, authorization, coding, billing, collections, and analytics. Physician billing services focus on the professional claims engine: coding, edits, submission, denials, posting, and reporting. Many vendors deliver both. You can engage billing services alone to fix targeted gaps and prove ROI fast.
How High-Performing Physician Medical Billing Services Work
1) Front-End: Eligibility and Authorization
- Verify active coverage, benefits, and referral rules.
- Confirm prior authorization for procedures, imaging, and injections.
- Capture medical necessity with problem lists, diagnostics, and failed therapy.
2) Accurate Coding and Smart Modifiers
- Select the right E/M level with current guidelines.
- Apply modifiers that drive payment accuracy: 25 (significant, separate E/M), 24/57 (timing), 59/XE/XS/XP/XU (distinct services), 26/TC (components), 76/77 (repeat), 95/GT (telehealth), and AI (principal physician).
- Ensure diagnosis specificity (ICD-10-CM) supports medical necessity.
3) Charge Capture and Reconciliation
- Reconcile schedules, encounters, and procedures daily.
- Tie documentation to charges (procedures, infusions, tests) so nothing drops.
- Audit no-shows, cancellations, and incident-to rules for NPPs.
4) Clean Claims and Timely Submission
- Submit claims within 24–48 hours of final documentation.
- Use payer-specific edits and LCD/NCD checks.
- Clear rejections within one business day.
- Track first-pass acceptance by provider and payer.
5) Denial Management and Appeals
- Categorize denials by root cause: eligibility/auth, coding, medical necessity, bundling, timely filing.
- Work denials within 48 hours using payer-specific appeal language.
- Trend issues, then update templates and checklists to prevent repeats.
- Share weekly denial scorecards with actions and owners.
6) Payment Posting and Underpayment Recovery
- Auto-post ERAs and match remit codes to contract terms.
- Flag short pays, MPPR reductions, and bundling errors.
- Send clean, patient-friendly statements with digital payment options.
- Track refunds and credit balances to protect compliance.
7) Reporting and Analytics That Drive Action
- Monitor clean-claim rate, initial denial rate, days in AR, net collection rate, charge lag, and >90-day AR.
- Break out performance by provider, location, service line, and payer.
- Share weekly wins and monthly executive summaries with next steps.
Physician Medical Billing Services by Specialty (Spokes)
Every specialty has hot spots. A strong partner knows them cold.
- Primary care and internal medicine:
- Annual wellness vs problem visits, CCM/TCM billing, vaccines, and G-codes.
- Cardiology:
- Global periods, diagnostic testing edits, and NCCI bundling.
- Orthopedics:
- Global packages, modifiers, and device/DME details.
- Radiology:
- Prior auth, component billing (26/TC), MPPR, and MUEs.
- Behavioral health:
- Telehealth POS, time-based coding, and payer parity rules.
- GI and surgery:
- Bundling, add-on codes, and post-op modifiers.
In-House vs Outsourced: Which Model Wins?
Both can work. Choose by scale, talent, and urgency.
- In-house advantages:
- Close clinical collaboration and quick clarifications.
- Direct control of workflows and staffing.
- In-house challenges:
- Recruiting certified coders for each specialty.
- Tooling costs, coverage gaps, and training load.
- Outsourced advantages:
- Scalable teams with deep payer nuance.
- Faster stand-up and lower fixed costs.
- Benchmarked KPIs and continuous QA.
- Outsourced challenges:
- Vendor selection and change management.
- Clear SLAs and data governance required.
When to Choose a Physician Billing Company
- First-pass acceptance under 95% or denials above 8–10%.
- Days in AR over 40–45 or >90-day AR above 20%.
- Frequent modifier or POS errors.
- Prior auth delays impact scheduling and cash flow.
- Documentation gaps block medical necessity.
What to Look For in a Partner
- Certified staff (CPC, CCS; specialty credentials a plus) and strong QA.
- EHR integration (Epic, athenahealth, eClinicalWorks, NextGen, Cerner).
- Payer-specific edit libraries; LCD/NCD mastery.
- HIPAA, SOC 2 controls, role-based access, and MFA.
- Transparent dashboards and performance-based pricing.
Tip: Ask for a live denial worklist demo and edit fire rates. Proof beats promises.
Pricing and ROI: What to Expect
Common pricing:
- Percentage of net collections (often 3–6%).
- Per-claim or project fees for backlogs.
- Hybrid models with incentives tied to clean-claim and denial goals.
Simple ROI view:
- Drop denials from 12% to 6% on $10M in annual claims. That 6-point shift can unlock hundreds of thousands after contract effects.
- Cut days in AR by 8–12 days. Faster cash reduces borrowing and bad debt.
Compliance and Security You Should Demand
- HIPAA training, BAAs, and PHI safeguards.
- SOC 2 Type II or equivalent audits.
- Encryption in transit and at rest, plus MFA.
- Role-based access, logging, and incident response.
- Coder accuracy audits with feedback loops.
30–60–90 Day Implementation Plan
Days 1–30: Discover and Baseline
- Connect EHR and clearinghouse; mirror work queues.
- Map denials by root cause; benchmark CCR, AR days, and charge lag.
- Set SLAs and reporting cadence; align on appeal templates.
Days 31–60: Stabilize and Improve
- Tighten edits, modifier logic, and medical necessity checks.
- Clear backlogs; rework high-value denials and short pays.
- Standardize prior auth and eligibility checklists.
Days 61–90: Scale and Optimize
- Launch provider scorecards and weekly revenue huddles.
- Train on documentation gaps and telehealth/POS rules.
- Lock continuous QA and quarterly payer-playbook updates.
Common Coding Pitfalls (And Fast Fixes)
- Modifier 25 use: Attach only to a significant, separate E/M on the same day.
- Telehealth: Use correct POS and modifier 95/GT per payer rules.
- NPP “incident-to”: Meet supervision and plan-of-care rules or bills under the NPP.
- Diagnostic tests: Link the right diagnosis to support necessity.
- Repeat procedures: Use 76/77 with supporting documentation.
Mini Case Insights
- Example 1: A multi-site primary care group raised first-pass acceptance from 92.1% to 97.8% in 60 days by tightening eligibility checks, modifier 25 use, and medical necessity links. Days in AR fell from 46 to 34.
- Example 2: A cardiology practice recovered $140k in a quarter after auditing MPPR reductions and short pays, then updating appeal templates and payer rules.
Tools and Integrations That Matter
- EHR/PM: Epic, athenahealth, NextGen, eClinicalWorks, Cerner.
- Clearinghouses: Availity, Waystar, Change Healthcare.
- Edits and QA: NCCI, payer bulletins, LCD/NCD updates.
- Analytics: Denial root-cause mapping, underpayment detection, provider scorecards.
Ask vendors to show live claim status, edit fire rates, denial turnaround, and short-pay recovery real data, not slides.
How to Measure Success
Track and publish weekly:
- Clean-claim rate: 95–98%.
- Initial denial rate: below 5–7%.
- Days in AR: under 40; >90-day AR below 15–20%.
- Charge lag: under 48 hours from encounter close.
- Net collection rate: 95%+.
- Auth turnaround: same day for urgent; <72 hours standard.
FAQs
What makes physician billing services different from hospital billing?
Physician billing services focus on professional claims (837P), E/M coding, and modifier logic. Hospital billing emphasizes facility claims (837I), revenue codes, and DRGs. Many groups need both, but the rules and edits differ.
Do you handle prior authorization?
Yes. We centralize auth for procedures, imaging, and injections, record validity windows, and verify medical necessity. These steps cut avoidable denials and scheduling delays.
Will you integrate with our EHR?
Yes. We integrate with major EHR/PM systems and clearinghouses, mirror your queues, and maintain secure, role-based access and audit trails.
How fast will we see results?
Most practices see cleaner claims and faster cash in 30–60 days. By 90 days, trend insights drive training and front-end fixes that compound results.
How do you protect PHI?
We maintain HIPAA compliance, sign BAAs, use encryption and MFA, and operate under audited controls (e.g., SOC 2 Type II). We log access and test incident response.





